 DVT – Blood Clots
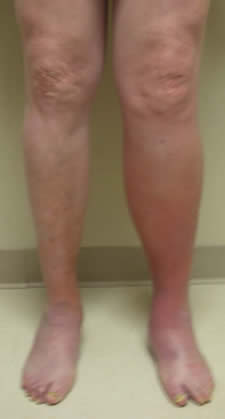
DVT – Blood Clots
Patients often remember a family member who suffered from blood clots. Blood clots can occur both in arteries and veins. Arteries carry blood from the heart to the tissues and veins return the blood from the tissues back to the heart. Both artery and vein clots are potentially dangerous but are different from each other in many respects. Only venous blood clots commonly referred to as DVT or DVT clots are explained below. DVT is an abbreviation for deep vein thrombosis. Thrombosis is the medical term for a blood clot.
Clotting of the blood is a necessary safety mechanism. It prevents a person from bleeding to death from a minor cut or everyday injury. The injured tissue produces a substance that promotes blood clotting at the site of injury.
Nature has provided several mechanisms to prevent blood from clotting inside the blood vessels. The movement of blood inside the blood vessels, itself, is a protective mechanism. Blood clots does not form unless there is stagnation of blood (“stasis”). However, stasis within veins can occur in patients who are inactive or bedridden. Muscle activity in the legs such as walking is necessary to keep the circulation going in veins. A form of this type of DVT clot sometimes occurs when patients travel long distances in a sitting position.
Most DVT blood clots occur in leg veins. Arms are less affected, as arm movements are maintained even in sedentary patients. The incidence of DVT blood clots is very high in patients who are very sick, such as those who are admitted to the intensive care unit in the hospital. Stasis can also occur in patients who are immobilized by plaster casts on the legs or restricted to bed by back problems, joint replacement, multiple fractures following a motor vehicle accident or other forms of injury. Often, tissue factors that promote blood clots following these types of injury add to the stasis problem to increase the risk even further. Stroke often confines the patient to bed for weeks or months, and leg muscle action may be impossible due to paralysis. The occurrence of DVT clots is high in these patients.
Several substances are present in the circulating blood that act against formation of a blood clot. Many of these molecules have been identified, but some are not identified yet. Some patients are deficient in one or more of these substances as a hereditary defect. The medical term for this condition is thrombophilia (Greek word for ‘prone to blood clot’) These patients are ‘hypercoagulable’– medical jargon meaning ‘prone to blood clots’. Some thrombophilia defects are more serious than others, so the risk of blood clots varies according to the type of defect. Factor V deficiency, also known as the Leiden gene defect is one such mild defect. It is present in about one in five individuals. Prothrombin gene deficiency is another such mild deficiency, which is also present in many individuals. The blood clot risk in these mild defects is only slightly increased over the general population. The risk of DVT clots is much higher in certain other forms of molecular deficiency.
There are several natural conditions, such as pregnancy that may increase clotting tendency. The risk is highest in late stages of pregnancy and during several weeks after childbirth. The risk of blood clots gradually increases with age. Some hormones and medications can also increase clotting tendency. The risk of DVT clots from birth control pills and estrogen replacement pills has greatly decreased because of better formulations, but some mild risk is still present. Some patients on these medications may develop DVT clots when a mild form of thrombophilia such as the Leiden gene or prothrombin gene deficiency is also present, increasing the risk.
Some diseases, particularly cancer, are a strong promoter of DVT clots. Vein problems, such as varicose veins or leaking valves in the deep veins, can also increase the risk of DVT clot formation. A DVT clot causes damage and scarring of the veins. This scarring produces narrowing of the veins. This, in turn, slows the movement of blood in veins causing stasis. Thus, a vicious cycle is produced where in which a previous DVT clot increases the risk of future DVT clots. Blood clots also function as irritants setting up inflammation of the vein, which compounds the scarring. For these reasons blood clots should be removed as soon as possible. There is a limited time to do this, however. Blood clots harden like cement with time. They may be so hard and stuck to the vein that it is not possible to remove them. Quick diagnosis and fast removal are recommended whenever feasible.
Roughly 6 out of a 1000 people develop blood clots every year. In most such cases, there is a well known cause for the blood clot such as a motor vehicle accident or one of the many conditions described above. These are known as provoked DVT clots. In a small percentage, the reason why the clot occurred is not clear. These are known as unprovoked DVT clots. Blood thinners on a permanent basis are often recommended for these patients.
Pulmonary Embolism
When a blood clot travels to the lung, it is called “pulmonary embolism”. A piece of a DVT clot that breaks away and travels with the circulation to another part of the body is known as an embolus. Most often this produces no symptoms at all or only mild to moderate symptoms such as shortness of breath. In a small percentage, perhaps 1 in 100 sudden death may occur. These are usually sick patients prone to blood clots for a variety of reasons described above. The traveling blood clot has to be large in size to produce death. Not all blood clots travel to the lung. Blood clots in the superficial veins such as varicose veins do not break easily to travel. Therefore, the risk of pulmonary embolism is very low. But they may cause intense pain and inflammation over the clot for two to three weeks. Blood clots from the arms also do not often travel to the lung. DVT clots in the deep veins of the leg are often silent—there is no pain or other indication that a DVT clot has formed. They are the ones that tend to travel to the lung. They are also large enough to cause death. It is estimated that 90% of blood clots that travel to the lung originate from deep veins of the leg. The treatment for blood clots in the deep veins of the leg is administration of blood thinners. This is also the main treatment for pulmonary embolism—clots that have already traveled to the lung. The lung has a great ability to dissolve clots that have travelled there if blood thinners are given for three to four months. In contrast, blood thinners do not dissolve DVT clots that are still in place in the deep veins of the leg. They do help to prevent the clot from growing larger and may help it shrink in size. Eventually, most DVT clots in the deep veins of the leg turn into scar tissue that narrows the vein.
In cases where blood thinners cannot be safely given because of bleeding risk from stomach ulcers for instance, filters (known as IVC filters) can be inserted above the clot to trap it if it tries to move. They are needed only temporarily, for example, for two months or so. By then the clot has turned into solid scar tissue within the vein and is not able to move. IVC filters should be removed as soon as they have served their purpose. This is because, IVC filters themselves can scar the deep vein after they have been in place for three months or more.
Scar tissue that is a result of a DVT clot in the deep veins of the leg generally causes no serious health problems. However, annoying symptoms such as leg pain, heaviness and swelling and occasionally even leg ulcers can develop from narrowing of the vein. This prevents healthy circulation in the legs. This is known as Post thrombotic syndrome– which literally means a symptom condition that develops after a deep vein DVT clot. Medical grade support stockings can be a great help in controlling these symptoms. In selected cases where compression stockings fail to provide relief, stents may be placed to open up the narrowed vein. Stents look like a large coil spring made of metal. They can be inserted into the vein through needle sticks.

